Leaky gut — or increased intestinal permeability, as it is known in clinical settings — has become one of the most discussed topics in functional medicine. While mainstream medicine has been slower to recognise it as a standalone diagnosis, the scientific evidence for the role of intestinal permeability in chronic disease is growing rapidly. Understanding what leaky gut is, what causes it and how to address it can be transformative for people struggling with unexplained symptoms.
What Is Leaky Gut?
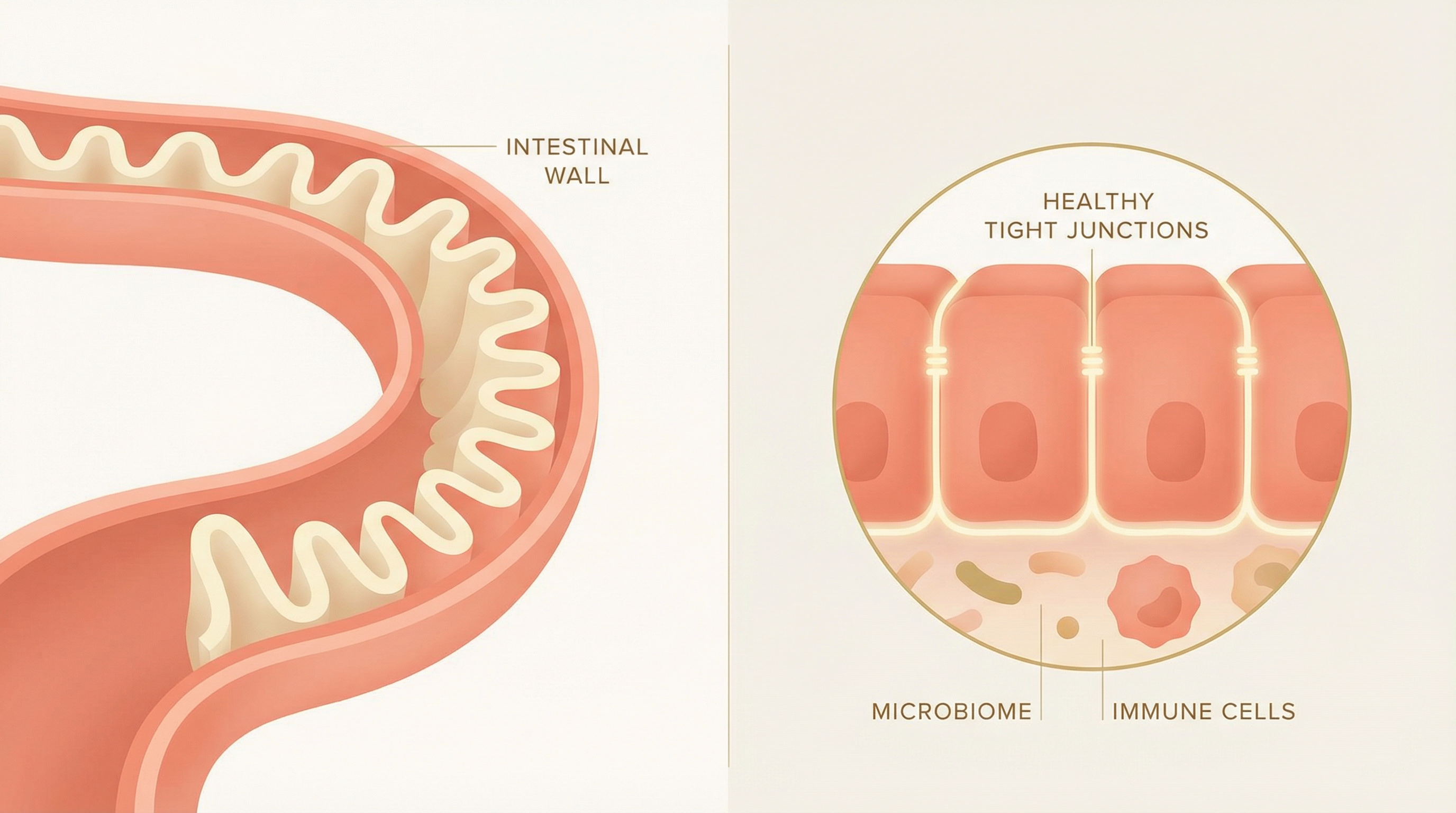
Your intestinal lining is a single layer of cells held together by structures called tight junctions. In a healthy gut, these tight junctions act as selective gatekeepers, allowing nutrients, water and electrolytes to pass into the bloodstream while keeping harmful substances — bacteria, toxins, undigested food particles — safely contained within the digestive tract.
When the tight junctions become damaged or loosened, the intestinal barrier becomes more permeable than it should be. This allows substances that would normally be contained within the gut to 'leak' into the bloodstream, triggering an immune response and systemic inflammation.
What Causes Increased Intestinal Permeability?
Multiple factors can compromise the integrity of the gut lining:
Chronic stress — Sustained psychological stress increases cortisol production, which directly weakens tight junction proteins and reduces blood flow to the gut lining.
Poor diet — Diets high in refined sugar, processed foods, alcohol and food additives (particularly emulsifiers such as polysorbate 80 and carboxymethylcellulose) have been shown to increase intestinal permeability.
Dysbiosis — An imbalanced gut microbiome, with reduced diversity and overgrowth of pathogenic organisms, produces inflammatory compounds that damage the gut lining.
Non-steroidal anti-inflammatory drugs (NSAIDs) — Regular use of ibuprofen, aspirin and similar medications is a well-documented cause of increased intestinal permeability.
Infections — Bacterial, viral and parasitic infections can damage the gut lining directly and alter the microbiome composition.
Excessive alcohol consumption — Alcohol disrupts tight junction proteins and promotes the growth of gram-negative bacteria that produce endotoxins.
Zonulin overproduction — Zonulin is a protein that regulates tight junction permeability. Gluten and certain bacterial exposures can trigger excessive zonulin release, opening the tight junctions.
Symptoms of Leaky Gut
Because increased intestinal permeability triggers systemic inflammation and immune activation, its effects are rarely limited to the digestive system. Common symptoms include:
Digestive Symptoms
- Bloating and gas, particularly after meals
- Abdominal pain or cramping
- Alternating constipation and diarrhoea
- Food sensitivities that seem to multiply over time
Systemic Symptoms
- Chronic fatigue and low energy
- Joint pain and muscle aches
- Skin conditions such as eczema, acne or rosacea
- Brain fog, poor concentration and memory difficulties
- Headaches and migraines
- Mood disturbances including anxiety and depression
- Frequent infections or slow recovery from illness
Associated Conditions
Research has linked increased intestinal permeability to a range of chronic conditions, including irritable bowel syndrome (IBS), inflammatory bowel disease (IBD), coeliac disease, type 1 diabetes, rheumatoid arthritis, multiple sclerosis and chronic fatigue syndrome.
How Is Leaky Gut Assessed?
In functional medicine, several approaches can help assess intestinal permeability:
Comprehensive stool analysis — Evaluates markers of inflammation (calprotectin, lactoferrin), digestive function and microbiome composition.
Zonulin testing — Elevated serum or stool zonulin levels indicate increased tight junction permeability.
Lactulose-mannitol test — Measures the ratio of two sugar molecules in urine after ingestion, providing a direct assessment of intestinal permeability.
Blood markers — Elevated lipopolysaccharide (LPS) antibodies or intestinal fatty acid-binding protein (I-FABP) can indicate barrier compromise.
A Functional Medicine Approach to Healing Leaky Gut
Restoring gut barrier integrity requires a systematic approach that addresses the underlying causes while supporting the healing process. The well-established '5R' framework provides a structured protocol:
1. Remove
Identify and eliminate the factors contributing to gut damage. This may include removing inflammatory foods (gluten, dairy, refined sugar, alcohol), addressing infections or bacterial overgrowth and reducing NSAID use where possible.
2. Replace
Support optimal digestion by replacing any deficient digestive factors. This may include digestive enzymes, hydrochloric acid (betaine HCl) or bile acids, depending on individual assessment.
3. Reinoculate
Restore beneficial bacteria through targeted probiotic supplementation and prebiotic-rich foods. Specific strains such as Lactobacillus plantarum, Bifidobacterium infantis and Saccharomyces boulardii have demonstrated gut barrier-supportive properties.
4. Repair
Provide the nutrients needed to rebuild the gut lining:
- L-glutamine — The primary fuel source for intestinal epithelial cells, typically supplemented at 5-10 grams daily
- Zinc carnosine — Supports tight junction integrity and reduces inflammation
- Omega-3 fatty acids — Reduce intestinal inflammation and support cell membrane repair
- Vitamin D — Essential for immune regulation and gut barrier function
- Collagen peptides — Provide the amino acids (glycine, proline, hydroxyproline) needed for tissue repair
- Butyrate — A short-chain fatty acid that nourishes colonocytes and strengthens the gut barrier
5. Rebalance
Address lifestyle factors that affect gut health, including stress management, sleep quality, regular physical activity and mindful eating practices.
Dietary Strategies for Gut Barrier Repair
Bone broth — Rich in collagen, glycine and glutamine, bone broth provides the building blocks for gut lining repair.
Cooked vegetables — Easier to digest than raw vegetables during the healing phase, while still providing essential nutrients and fibre.
Healthy fats — Olive oil, avocado, coconut oil and oily fish provide anti-inflammatory fatty acids that support cell membrane integrity.
[Fermented foods](/resources/articles/fermented-foods-benefits/) — Introduce gradually to provide beneficial bacteria without overwhelming a sensitive gut.
Avoid common irritants — During the initial healing phase, reducing or eliminating gluten, dairy, refined sugar, alcohol and caffeine can significantly accelerate recovery.
How Long Does It Take to Heal?
The timeline for gut barrier repair varies depending on the severity of damage, underlying causes and individual factors. Many people notice improvements in digestive symptoms within 4-6 weeks of implementing a targeted protocol. Full restoration of gut barrier integrity typically takes 3-6 months, though some individuals with long-standing permeability issues may require longer support.
The Bottom Line
Leaky gut is a real and measurable condition with far-reaching effects on health. If you are experiencing a combination of digestive symptoms and systemic complaints that conventional medicine has not been able to explain, increased intestinal permeability may be a contributing factor. A functional medicine approach that identifies the root causes and supports systematic healing can help restore gut barrier integrity and resolve symptoms throughout the body.